By Namiganda Jael
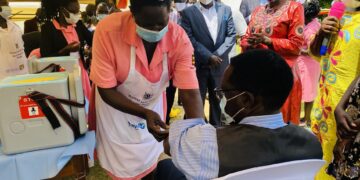
Sister Lekuru Joyce Judith, a senior assistant nursing officer palliative care at st. Kizito Matany hospital, is from visiting a cancer patient under an outreach program run by the hospital in Napak district Karamoja sub region. She has to travel 10 kilometers for every visit to tend to her 60 year old patient who suffers from colon cancer.
Her patient Biiru Florence depends entirely on her for any medical and psycho social support. Sister Lekuru travels hundreds of kilometers every month to bring supportive treatment and counselling to her patients who would otherwise not receive any medical care whatsoever.
Biiru says, before, her family could hardly raise the funds to meet the expenses she needed to visit a major hospital, approximately 250 miles away in Kampala, for chemotherapy however, this changed when sister Lekuru visited and subsequently did follow up on her case while providing her with all the supporting treatment she needed.
“I am now actively following up on all my treatment and counseling sessions, despite the cancer, I feel alive unlike before when I even had suicidal thoughts,” she says smiling.
Clare Nyakwer, Biiru’s daughter and only caretaker says her mother is more vibrant now and looks towards living longer because of the care she has been receiving for the past one year under sister Lekuru.
“My mother had given up any hope and had even asked me to suffocate her because she could not bare the pain yet we couldn’t afford any form of treatmet, but sister Lekuru provides us with pain medications especially morphine and some times even food because hunger is a problem in this area,” she explains.
According to Dr. Muwanga Moses, the assistant commissioner clinical services under palliative care at the Ministry of health, over 40 million world over need palliative care services with the developing world like Uganda accounting for 70% of these.
He explains that palliative care is the total care provided to people with chronic illnesses such as cancer, diabetes, sickle cells and hypertension among others.
“It starts immediately a diagnosis is made and goes all the way, because a time reaches when therapeutic therapy is no longer important and people need palliative care,” he notes.
Mark Donald Mwesiga, Executive officer, Palliative Care Association of Uganda (PCAU),says palliative care is the holistic care for individuals who are faced with health related suffering and conditions that comes to someone through professional or medical attention, in terms of an injury from accidents or disease causing one suffering to the extent that it is life limiting and limits one’s ability to live life as before, or have it to the point of death.
He explains that palliative care addresses four areas which include physical pain where one experiences pain in the body such as cancer and social pain which comes with a social impact on family and marriage as well as the community.
The other areas it addresses is spiritual, where one starts to question God and their entire existence with questions like, God why me? and the psychosocial area where the mental ability for someone to go through the condition is affected. This is taken care of with counselling and psychosocial support by professionals who can address all these areas to lessen the burden and pain.
Palliative care, which was introduced by Hospice Africa Uganda in 1993, is now being integrated in to Uganda’s health structures as a major medical and therapeutic area especially for remote inaccessible villages deep in Karamoja subregion. Since the project began in the sub region in 2010, it has cared for well over 10, 000 families.
The care given is holistic including medical, social, emotional, psychological and spiritual, to both the patient and their family. Most families prefer to nurse their loved ones at home especially those in remote areas.
Biiru is not the only patient who had given up on life, 20 kilometers away from her home in Moroto at Loptuk village, in Loptuk parish Nanduget subcounty is Moses Achia who is on his way to full recovery after he suffered a stroke that left his left side paralyzed.
Achia can now move on his own without any support thanks to the psycho social and physiotherapy support he received from sister Lekuru and her team. Achia was rushed to Nanduget health centre IV where he received treatment and this is where the palliative care team from Moroto referral hospital found him. He has since been cared for by the team.
“We were in a community out reach programe at the Nanduget community centre where we met Achia’s wife Annet. She told us about her husband’s state and we visited him, he was in a terrible state. We then embarked on a mission to make him better, even after he was discharged from the health centre, we did follow up at home and enrolled him on our full palliative care package,” says Juliet Acidri a health volunteer under palliative care department at Moroto hospital.
Acidri says she and her team have offered palliative care services to Achia at the comfort of his home for two years now, visiting at least twice a month. “He is now able to do most things by himself unlike before when he had no special care,” says Annet, his wife.
Sister Lekuru notes that they are currently following up over 426 patients in Nanduget alone, where they started with just two in 2010. In addition to the three professionals, they have over 500 volunteers on the village health teams in Moroto, this is a growth from just 50 volunteers in 2010.
Their work typically involves visiting the patient’s home, giving them psycosocial support and painkillers like morphine twice a month. However, depending on the severity of the case, follows up are done on a weekly basis.
Dr. Muwanga reveals that through the Ministry of health, the Government of Uganda has made it a point to include palliative care services under all regional referral hospitals. “Before over 40 districts lacked a single palliative care department as well as health service providers specialized in palliative care but government is working hand in hand with associations like PCAU to ensure that more providers are trained to provide these services,” he adds.
Dr. Muwanga notes that all national referrals including Mulago and Butabika, as well as all regional referrals and general referrals are now offering palliative care and making morphine readily available at a free cost.
Mwesiga says palliative care has moved a very long way since it’s inception due to the commitment of all players with services such as the free access to medicines provided by the government of Uganda (oral liquid morphine, essential for management of severe pain), education where students can now access a diploma, degree or masters in palliative care with over 120 professionals trained so far, the Policy framework where the National Palliative Care policy is in the offing and finally Integration of palliative care services in the public health care structure, up to health center 4 level.
According to him, there are over 226 public health facilities which have a palliative care service unit distributed across 107 districts in 2022 as compared to 2010 where only less than 20 units were providing service and only facilitated by non- governmental organizations.
Mwesiga says the biggest challenge they face now is that there is still a huge gap to be bridged in some hard to reach areas where palliative care services have not reached and subsequently many people have to move long distances to access the services in the districts where they are provided.
Sister Lekuru also notes that accessibility is the biggest challenge they face. “Most of the care is in the community and homes, we visit our patients at home in the villages. The biggest challenge is accessibility as many stay very far away. This is a big challenge as only 17% of the people stay within the recommended area of five kilometers meaning that 83% of the people in need of the service stay very far,” she says.
Inadequate manpower is also a challenge. Sister Lekuru says that at St. Kizito Matany hospital, a palliative care unit was established in 2015 following a government facilitated training but there are only three trained professionals in palliative care. Thus, they have to work with volunteers yet they serve huge populations in Karamoja sub region, Iteso, Bugisu and sometimes as far as western Kenya.
She adds that as palliative care service providers, they are required to be honest with patients and care takers but whenever they open up to families especially about cancer, some care takers abandon the patients in the hospital or in homes.
Sister Lekuru also identifies alcoholism and substance abuse as another major challenge they face while providing palliative care services as most patients under palliative care have liver problems due to heavy alcohol consumption. “Alcohol consumption with most patients and clients is killing many before their time, we do our part with the counselling and all but this addiction is becoming a major stumbling block,” she notes.
Additionally, the hospital used to work with radio stations in Moroto who offered free space for one and half hours per week for them to mobilize the communities to embrace palliative care services through educational programs which were interactive with call in opportunities. However, the radio stations now offer very limited space of just 30 minutes per week yet the hospital has many programs under different departments, Sister Lekuru says.
Additionally, she points out that people are mobile and keep changing location, saying, “they keep moving, today you visit a patient in one place and next time you go they have moved.”
According to Dr. Muwanga, despite the support Hospice Africa and community leaders have provided, there is still a challenges of patients and caretakers opting to seek services from traditional healers. He however says, they are now working with local leaders, traditional healers themselves and religious leaders to educate the public and bring about a mindset change and for traditional leaders to always refer them to hospitals where they can access proper diagnosis and palliative care services.
He says for the challenge of transportation, the ministry of health is now mobilizing funds to buy motorcycles for health workers to easily access these areas in the next financial year.
Dr. Muwanga also promises that government is currently working on formulating a policy regulating palliative care services ( the national palliative care policy). he notes that “as government, they are working to ensure that all our health workers are trained and facilitated in terms of palliative care because there’s need for a proper regulatory frame work for the palliative care services in Uganda. He calls on those with patients with need of the services to seek help instead of sitting on them at home especially those with chronic illnesses such as cancer.”