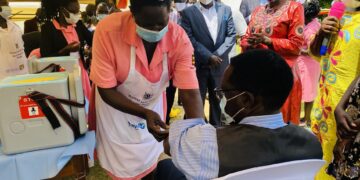
With a total of 9800 preterm deaths annually in Uganda, health practitioners have stepped up their efforts to reduce these alarming statistics numbers to an acceptable figure.
The World Health Organization (WHO) recommends that children born with very low birth weight of less than 2.5kgs who are estimated at 20 million worldwide be initiated on human breast milk immediately to boast their immunity and avoid retarded growth. Dr. Victoria Nakibuuka, a neonatologist at Nsambya Hospital and head of the paediatric Unit says
Nsambya Hospital has adopted a no formula policy and emphasized donation and recipient of breast milk at the facility in a bid to reduce malnutrition and health complications in babies that might arise at their earliest stages in life.
Dr Nakibuuka says that this resolution is being mooted as a solution to the challenges faced by preterm mothers who fail to feed their children because they lack milk at the time.
“We have a no formula policy so we encourage mothers with more breast milk to donate milk to those who have not generated theirs especially those with preterm or with multiple babies so that their babies can have a healthy start to life coupled by getting all the nutrients they need in their early stages of life.” Dr. Nakibuuka notes.
She says that they are currently doing the breast milk banking at a small scale, local basis with a minimal 2 to 3 mothers donating milk on a daily, depending on the demand but she’s optimistic that it will expand when the equipment for the bigger bank arrive.
“We are currently receiving two to three mothers a day or after a few days depending on the need. However, when the machinery which was delayed due to the COVID 19 pandemic arrives, we hope to utilize the bigger bank which is expected to be opened in August or September this year. We are also going to collaborate with other bigger hospitals like Mulago and Rubaga to ensure all new babies born access breast” Dr. Nakibuka adds.
Ms. Persis Lule, a mother of four preterm babies, says she could not feed her babies; she was advised to get a donor because she couldn’t feed her babies herself as she could not generate enough milk for them all. Persis then had to solicit for donors to ensure that her preterm babies still in NICU would be well fed as the hospital has a strict no formula policy for preterm babies.
“Since I was a caesarean mother with preterm babies my body was a little stressed to produce breast milk for my four babies who were in NICU but after the doctor talked to us about receiving breast milk from a donor, I was able to receive breast milk from a friend I trusted who had also just given birth and were able to receive about 150mls of milk.” Persis adds.
Access to donated breast milk by neonates is anticipated to reduce the number of neonatal deaths that are now estimated at 27 per 1000 live births.
Sister immaculate Nabwami, who is in charge Neonatal Unit at Nsambya hospital, says they sometimes get an overwhelming number of preterm babies who need the donated milk and the demand becomes higher that the supply which gets frustrating as they strive to keep these babies alive and on course.
For this, she says, they tend encourage mothers who have more than enough milk for their babies to donate the milk. She adds that mothers with preterm babies usually lose breast milk, majorly because their bodies have not yet adjusted, others have more babies, or some are stressed becauseof the hospital bills.
Breast milk donors undergo some tests for diseases such as HIV/Aids, syphilis, and hepatitis, to ensure that the milk is safe.
Ms. Fariuz Naiga, who was admitted in Nsambya hospital for three months after the delivery of a premature baby, says she had plenty of milk but her baby took too little because it was very small,.
After hearing about the hospitals no formula policy and the breast milk bank by the facility, she decided to donate some of her milk which was in excess to mothers who had given birth to multiple babies and were in dire need of much more milk at the time.
“I underwent tests which the recipient mothers paid for and after the tests came back negative, I was able to donate the milk at free will and every time I brought milk for my baby part of the milk went to the mothers one of whom was a mother whose triplets were underweight” she adds.
Dr. Sabrina Kitaka a pediatrician at HIV clinic of Baylor Uganda said breast milk banks are very helpful even for mothers living with HIV noting that while breast feeding for six months is recommended for them, they still fear many are not adhering to their medication.
Dr. Nakiibuka stressed that they still face a challenge of substandard equipment as they mostly operate at a more manual basis. She is, however, hopeful that more funding will come through when the bigger bank is commissioned. “For now, we keep the donated breast milk in ordinary fridges and warm the milk with just hot water locally but hope for more funding so that we use updated equipment and get the bigger bank fully operational” she noted. She further stresses that the project is entirely dependant on funding and fundraising.
Uganda’s health ministry records indicate that up to 9,800 premature babies die in Uganda annually but it is estimated that increased breastfeeding could also avert an estimated 20,000 deaths each year due to breast cancer globally.
Dr. Nakibuuka says she is now championing an awareness campaign to all mother’s able to donate to always consider donating to save the lives of many preterm babies who may stand no chance at all especially in remote villages away from Kampala. She also calls on donor partners to come on board and make the breast milk donation campaign a nation-wide drive just like the blood donation campaign.
She further encourages leaders at various levels, especially the health ministry, to address this need at a policy level, for every child deserves a chance at life.